What Really Works (Based on What I've Seen)
Although stress management and burnout prevention techniques are universal, the nursing profession has nuances that require a distinct approach. Here's what I've learned actually helps when you're drowning in stress and feeling like you can't keep going:
- Thirty-second resets during your shift – The 4-7-8 breathing thing works. So does turning handwashing into a mindful moment. These aren't just feel-good suggestions…they actually activate your parasympathetic nervous system between patient interactions.
- Your EAP is there for a reason – Some nurses don't even know they have access to free 24/7 counseling through their workplace. The productivity improvement alone can be worth $15,600 annually, but more importantly, it's confidential support when you need it.
- Push back on the system – I know this feels impossible, but advocating for better staffing ratios and actual break policies matters. Each additional patient per nurse increases your risk of burnout by 23%. That's not just a statistic – that's your mental health.
- Find your people at work – Structured peer support programs reduce depression and increase empowerment. Working under leaders who give you autonomy and actually recognize your work makes a massive difference.
- Make boundaries non-negotiable – Over 60% of nurses globally struggle with work-life balance. This isn't a personal failing…it's a professional epidemic that requires you to get serious about time management and self-care.
What I've discovered is that individual tools only work when the organization you work for gives a damn too. You need both personal strategies and systemic support. Otherwise, you're just putting band-aids on a system that's actively burning you out.
Why This Matters to Me
Burnout in nursing hit home for me during my recent annual physical. The nurse who greeted me kindly let me know that she was happy to see me because I “bring good energy” to an office where it's “one thing after another.”
That conversation reminded me why I do this work as a Certified Corporate Wellness Specialist® and mental health speaker. The reality is stark: 62% of nurses experience burnout [51], with younger nurses under 25 facing even higher rates at 69% [51]. What's more concerning is that each departing bedside nurse costs approximately $61,000 in turnover [51].
As someone who delivers presentations at nursing conferences and healthcare organizations, I've seen firsthand how much nurses are struggling. You deserve practical tools that actually work in real-world clinical settings, not just wellness advice for your days off.
What Nurse Burnout Really Looks Like (And Why 2026 Is Different)
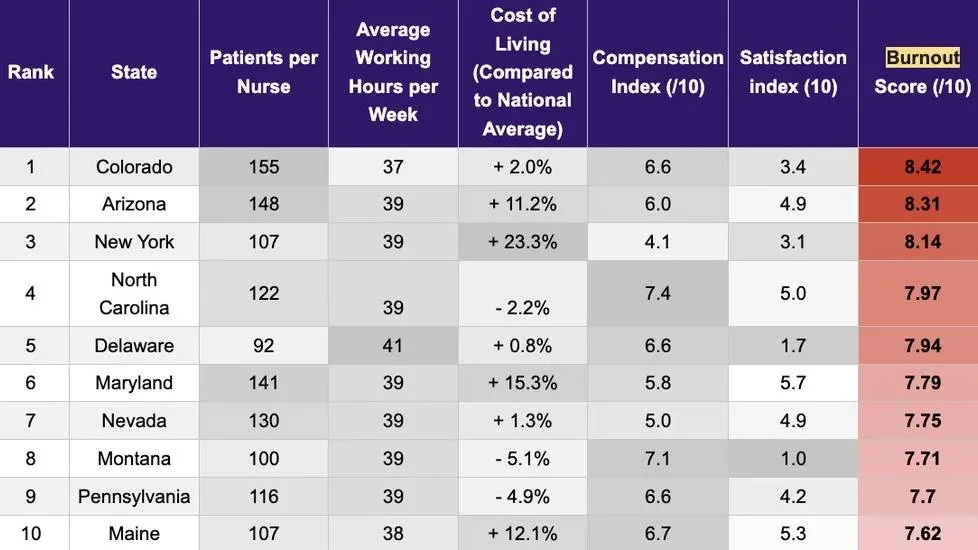
Image Source: Nurse.org
Here's What We're Actually Dealing With
The World Health Organization finally got honest about burnout. They put it in the International Classification of Diseases (ICD-11) as an occupational phenomenon, not a medical condition [1]. I like that distinction. It acknowledges this isn't about individual health.
The official definition describes burnout as a syndrome from chronic workplace stress that hasn't been successfully managed [1]. Three specific dimensions: energy depletion or exhaustion, mental distance from your job with cynicism, and reduced professional effectiveness [1]. This framework applies specifically to work contexts, not your entire life [1].
Here's what I see at nursing conferences: These three dimensions hit nurses especially hard. You're making life-or-death decisions in high-stress settings [2]. Long hours, pressure to make quick decisions, and emotional strain from caring for patients who may not make it [2]. When these factors pile up, disengagement and detachment show up first [2].
What makes 2026 different? We're finally admitting burnout is a workforce crisis with real effects on patient outcomes [3]. The conversation shifted from “build individual resilience” to “fix the broken systems.” The Joint Commission now recommends that healthcare organizations focus on meaningful work, nurse goals, and professional autonomy rather than just teaching coping skills [3].
About time, honestly.
The Numbers Don't Lie (And They're Getting Worse)
I spend a lot of time looking at burnout data for my presentations. The current numbers are brutal.
AMN Healthcare's 2025 survey found 58% of nurses report feeling burned out most days [3]. Only 39% plan to stay in their current position within the next year [3]. That means nearly two-thirds of working nurses are already considering leaving [3].
More stats that are problematic:
- 65% of nurses are experiencing stress and burnout
- Over 50% feel unsupported at work
- Nearly 60% believe leadership prioritizes profits over patient care [51]
The workforce loss is real. More than 138,000 registered nurses have left since 2022 [51]. By 2029, almost 40% intend to leave [51]. Among nurses who actually left their jobs, 31.5% cited burnout as a reason in 2018 [5]. For those considering leaving, 43.4% identified burnout as a factor [5].
The trend over time tells the story: 30.4% in 2018, 31.3% in 2019, 30.9% in 2020, 35.4% in 2021, 39.8% in 2022, and 35.4% in 2023 [51]. Burnout stayed relatively stable until the pandemic hit, then jumped significantly in 2021 and 2022 [51]. Even with a decrease after COVID-19's official end in May 2023, burnout remained 16.4% higher than the first year studied [51].
IMPORTANT: Different specialties get hit differently. ICU nurses report the highest rates of low personal accomplishment. Oncology nurses have the highest rates of depersonalization [3]. A study in Psycho-Oncology found that 30% of oncology nurses reported emotional exhaustion, while 35% reported feelings of low personal performance [2]. Primary care physicians had burnout levels ranging from 46.2% in 2018 to 57.6% in 2022 [51].
Age makes a huge difference. Younger nurses under 25 reported burnout rates of 70%, compared with 40% among those over 55 [6]. In Sweden, 20% of newly graduated nurses showed burnout symptoms in their first three years [51]. Among those with burnout symptoms, 27% intended to leave after 1 year, 45% after 3 years, and 43% after 5 years [51].
What Burnout Actually Looks Like (Don't Ignore These Signs)
Physical exhaustion that persists even after rest. This isn't surprising, given that 30% to 70% of nurses get less than 6 hours of sleep before 12-hour shifts [51]. Only 27.2% got at least six hours of sleep before shifts, and 29.1% of shifts were worked by nurses with less than six hours of sleep [2]. Chronic fatigue leads to reduced job satisfaction, decreased productivity, and increased error risk [4].
Emotional symptoms hit hard: cynicism toward work, panic about going to work, lack of empathy for patients [51]. You start withdrawing from relationships, your work ethic declines, and you respond more slowly to workplace requests [51]. Increased irritability toward patients and co-workers signals that your emotional reserves are running low [51]. Compassion fatigue becomes common – decreased empathy and emotional exhaustion from regularly caring for suffering or traumatized patients [4].
When anxiety becomes overwhelming, routine changes feel insurmountable. It interferes with eating, sleeping, and concentrating [4]. You lose enthusiasm for work, dreading shifts you once found fulfilling [4]. Physical consequences include weakened immunity, gastrointestinal issues, chronic pain, and heart palpitations [4]. These make you more vulnerable to illness and health complications [4].
Burnout affects your actual job performance. Difficulty concentrating or making decisions. Dread or apathy about work, procrastination, and avoiding once-routine tasks [51]. This can lead to patient care or documentation errors with serious consequences [51]. Chronic lateness and absenteeism become patterns – illness, fatigue, or mental health reasons for missing shifts [51]. At least 25% of health and care workers reported anxiety, depression, and burnout symptoms between January 2020 and April 2022, with no significant reductions since [9].
If any of this sounds familiar, you're not alone. And you're not weak.
What Really Works for Stress When You're on the Floor
The nurse who greeted me at my annual physical wasn't wrong when she said the workload feels relentless. After speaking at dozens of nursing conferences, I've heard this same story over and over. Nurses are operating in a constant state of stress activation, and it's literally changing their bodies.
Here's what happens: when stress becomes unrelenting, cortisol stays elevated through the hypothalamic-pituitary axis, creating a pro-inflammatory state that's linked to cardiovascular disease, immune dysfunction, and mental health conditions [51]. Since the pandemic, stress and burnout rates among healthcare workers have risen dramatically, affecting over three in every five workers [51]. Long hours, watching people suffer and die, unpredictable schedules, endless paperwork, and having zero control over your work conditions – it's the perfect storm for your stress response system to get stuck in overdrive [51].
That conversation with the nurse reminded me why this matters so much. She mentioned being grateful for patients who bring good energy because everything else feels like “one thing after another.” This is why you need practical, evidence-based techniques you can actually use during your shifts, not just wellness advice for your days off.
Chronic stress screws with way more than your mood. When your stress levels stay elevated without proper recovery, it disrupts cortisol regulation, trashes your immune function, and contributes to emotional exhaustion [51]. As healthcare workers, you put everyone else's well-being first, often delaying help for your own health needs [51]. Add the stigma around mental health treatment in healthcare, and you've got another barrier to dealing with stress effectively [51].
Two-Minute Fixes That Actually Work
I get asked this question at every conference: “What can I do when I only have two minutes?” Here's what the research shows – even micro-meditations of 30 seconds to 2 minutes create lasting changes in your body [51]. Just three deep breaths can measurably change your heart rate variability within 30 seconds [51]. When you make your exhale longer than your inhale, you're sending a direct signal to your brain that activates your parasympathetic nervous system, which slows your heart rate, lowers blood pressure, and reduces stress hormones [51].
- The 4-7-8 Reset takes 30 seconds: breathe in through your nose for 4 counts, hold for 7 counts, breathe out through your mouth for 8 counts, then repeat 2-3 more times [51]. That long exhale flips your parasympathetic nervous system on almost immediately [51]. There are actual nerve cells in your brain that connect breathing to your state of mind, and changing your breathing patterns can shift your relaxation, attention, and anxiety levels [52].
- The Two-Minute Body Scan is perfect for those transition moments. Start at the top of your head, notice whatever you feel without trying to fix anything, and slowly move down through your body, just acknowledging tension or relaxation as you find it [51]. T
- The Anchor Breath works when chaos is happening around you: pick one aspect of breathing to focus on, and when your mind starts racing, gently bring it back to your chosen anchor for 1-2 minutes [51].
- Mindful Handwashing gives you a 30 to 60-second reset. Instead of rushing through it, use handwashing as a moment to reconnect with your body and mind by focusing only on the sensations [53].
- Progressive Muscle Relaxation means consciously tensing muscles and then systematically releasing that tension, starting with your feet and working up through your body [52].
Building Real Resilience
Mindfulness-based interventions help nurses feel valued while actually reducing stress and improving work quality [54]. These are relatively low-cost interventions that work in various healthcare settings [54]. Mindfulness reduces depression and anxiety, helps regulate emotions, increases your ability to show empathy and compassion, and helps you cope with burnout [53].
There's a program called Mindfulness in Motion that's specifically designed for healthcare workers. It's an eight-week, evidence-based program that teaches practical techniques for reducing burnout and stress [54]. They offer group sessions that include teaching, community discussion, mindfulness, and gentle yoga. This program consistently delivers significant reductions in healthcare worker burnout and perceived stress, with real increases in resilience and work engagement [54]. They even measured biological stress markers, such as salivary α-amylase and plasma cytokines, and those decreased too [54]. Since 2017, over one thousand healthcare workers have completed this program, and many report benefits both personally and professionally [54].
Mobile mindfulness apps work well for nurses because you can do quick meditations or breathing practices during your clinical day [54]. Having it on your smartphone means you can access it during work and personal time [54]. The key is daily practice to condition your nervous system [55]. Nurses who regularly do mindfulness, self-care, and self-compassion seem more resilient to stressors and burnout [56].
Making It Work When Everything's On Fire
When everything is on fire, use the STOP technique.
The STOP technique is simple: Stop and pause whatever you're doing, take a breath, focus only on breathing, observe what's happening inside or around you, then resume what you were doing [57]. Some providers use a “STOP sign” approach during emergencies: Stop, Take a breath, Observe, and Priority first [58].
I know taking breaks for self-care while on shift seems impossible, but it's essential [27]. Focusing on your breath for a minute or two can foster self-awareness and bring you into the present moment [27]. You can sit for two minutes at the nurses' station or stand at your workstation [27]. Try affirmations such as “All that I do today is the best that I can do, and it's OK” to help restore a sense of centeredness [27].
Chair yoga and desk stretches can relieve tension in your back, neck, and shoulders in five minutes [56]. Taking even a few seconds during your shift to stretch your arms, legs, shoulders, or neck increases blood flow and potentially relieves stress [59]. If you work on the ground floor, step outside for a few minutes to get some fresh air [59]. Studies on the Japanese practice of Shinrin Yoku show that stress hormones decrease, people take deeper breaths, and the mind settles when exposed to nature [59].
The courses I recommend at nursing conferences include two-minute self-care practices, chair yoga techniques for desk-based movement, short meditations, and one-minute leadership tools. These give you practical options you can use immediately. The feedback I get from nursing staff always emphasizes that you need leadership support to make well-being work… mindfulness techniques could be seamlessly integrated into the clinical workflow if organizations actually backed it [54].
The Reality About Workplace Culture (And Why Most “Team Building” is Bullshit)
Through my work speaking at nursing conferences, I've witnessed firsthand how leadership can either save nurses or destroy them.
I've been in hospitals where charge nurses act like dictators and others where they genuinely care about their staff's mental health. The difference is night and day.
Leadership That Actually Prevents Burnout (Not Just Talks About It)
Leadership presence and conduct remain the most potent factors in every work setting [60]. Head nurse leadership plays a significant role in decreasing job burnout through two mechanisms: managing job demands and providing adequate job resources [60]. When leaders demonstrate effective techniques, nurses perceive a more supportive work environment that helps them cope with work-related stress [61].
Here's what I've learned from observing hundreds of healthcare leaders:
Transformational leadership and authentic leadership emerged as the most protective styles against burnout in nursing [61] [62]. But what does that actually look like in practice?
I've seen transformational leaders who emphasize individualized support, visionary inspiration, and ethical modeling, which enhances team cohesion through trust-building and goal alignment while fostering psychological resilience [60]. These are the managers who remember your name, ask about your family, and actually fight for better staffing ratios.
Authentic leaders serve as role models, fostering trust and supporting nurses, creating transparent interactions that promote professional growth [62]. They're the ones who admit when they don't know something and who take responsibility when things go wrong.
Conversely, abusive leadership was linked to increased burnout [61]. I've witnessed this too many times – managers who throw staff under the bus to protect themselves.
Effective leadership shows up as granting nurses autonomy, exhibiting compassion and empathy, and ensuring adequate nurse-patient ratios, which reduces stress and physical burdens while improving job satisfaction [60]. High-quality leader-member relationships, coupled with leaders' support and appreciation, help nurses reframe challenges and improve job satisfaction [60].
Building Real Peer Support (Not Fake “We're All Family” BS)
I'm tired of hearing about workplace “families” that don't actually support each other when things get tough.
Peer support programs help reduce perceived stress and mitigate stress-related physiological symptoms [63]. These programs match requestors with trained supporters from similar clinical backgrounds, which aids effective communication [63]. The keyword here is trained – not just assigning someone randomly.
Trained peer supporters listen to nurse concerns but don't offer advice unless requested, creating a psychologically safe space for active listening [63]. This isn't about fixing everything. Sometimes you just need someone who gets it.
The EmBRACE program at Emory Healthcare offers nurses an online platform accessible via email, URL link, or QR code [63]. Once matched, a trained peer supporter emails or calls the nurse to schedule a 45-minute conversation, with up to three sessions available for a specific concern [63]. Engagement in peer support reduces feelings of depression and increases feelings of empowerment and self-efficacy [63].
What makes this work? Peer support isn't therapy; it isn't judgmental, and it occurs confidentially in one-on-one settings [63]. The literature suggests that when team members feel psychological safety, quality and patient safety increase [63]. MedStar Health serves as a national leader in active nurse peer support programs [63].
Recognition That Actually Matters
Let me be honest about recognition programs – most of them suck.
Pizza parties and “Hero of the Month” certificates don't pay bills or reduce stress. Meaningful recognition acknowledges the value of individuals' professional contributions to an organization's work [64].
Here's what nurses actually want: Salary was the most valued form of recognition, followed by private verbal feedback and written acknowledgment [64]. Unlike earlier studies, professional development opportunities were the least valued form of recognition, reflecting a shift in nurse preferences [64].
Translation: Pay people fairly and tell them they're doing good work. It's not complicated.
Healthcare organizations need comprehensive systems that include formal processes and structured forums, ensuring sustainable focus on recognizing all team members for their contributions [65]. Recognition systems should reach from the bedside to the boardroom, ensuring individuals receive recognition consistent with their personal definition of meaning and fulfillment [65].
Peer-to-peer recognition programs promote camaraderie, respect, and collaboration, allowing staff members to nominate peers for specific accomplishments or acts of kindness [66]. When recognition comes from colleagues who understand the work, it carries more weight.
Communication That Doesn't Kill People
Communication breakdowns are identified as the primary root cause of treatment delays in the healthcare environment, reported 86 percent of the time [67]. These errors are also recognized as the chief root cause of infection-associated events, reported 75 percent of the time [67].
This isn't just about being nice – when healthcare professionals aren't communicating effectively, patient safety is at risk for several reasons: missing critical information, misinterpretation, unclear orders, and overlooked changes in status [68].
I've been in hospitals where nurses are afraid to speak up to doctors. I've also been in places where everyone communicates openly without fear of retribution. Guess which ones have better patient outcomes?
Effective teams are characterized by trust, respect, and collaboration [68]. Creating opportunities for different groups to get together is a highly effective strategy for enhancing collaboration and communication [68].
Simple fixes that actually work: encouraging open dialog, collaborative rounds, implementing preop and postop team briefings, and creating interdisciplinary committees reduce the likelihood of disruptive events [68]. Clear communication ensures that all staff know and can efficiently follow protocols and procedures, enhancing overall operational efficiency [69].
The bottom line? Good workplace culture isn't about fancy programs or motivational posters. It's about treating people like human beings and creating systems that actually support them.
Finding Balance When Your Job Demands Everything
Work-Life Balance Isn't Just Nice to Have – It's Essential
I used to think work-life balance was something other people worried about. Nurses? They just worked. They showed up, did their jobs, went home exhausted, and repeated the cycle.
That thinking nearly destroyed me.
Over 60% of nurses globally experience poor work-life balance, and honestly, I'm surprised it's not higher [70]. When I speak at nursing conferences, I see the exhaustion in people's faces. In Jordan, 72% of nurses report struggling with work-life balance due to long hours, heavy patient loads, and no personal time [70]. The consequences aren't just personal – increased burnout, high turnover rates, and compromised patient care quality all stem from this imbalance [70].
Here's what I've learned: employees who achieve equilibrium between work and personal life report less stress and greater job satisfaction, which in turn leads to better mental health outcomes [71]. Work-life balance directly connects to job satisfaction and inversely relates to psychological distress [71]. When nurses experience balanced work-life, they develop higher psychological capital, which improves mental health and job satisfaction [71].
The math is simple. The execution is hard as hell.
Setting Boundaries (And Actually Keeping Them)
Boundaries felt impossible when I started working with healthcare teams. How do you say no when someone's life depends on you?
But here's the reality: taking care of your physical and mental health helps you maintain professional boundaries [72]. Fatigue, stress, and burnout blur these lines, affecting your ability to provide objective patient-centered care [72]. The ability to say no to certain demands on your time and attention, or step away from situations that have become emotionally or physically taxing, is fundamental to performance [73].
I've watched nurses who articulate and enforce boundaries shield themselves from burnout. They recuse themselves from cases or patient needs that push them beyond their limits [73]. By reducing burnout, these nurses build resilience and stay in active practice longer [73].
Setting boundaries also involves educating patients and their families about what they can expect from nursing care. This fosters understanding and helps them align expectations with healthcare delivery realities [74].
Time Management When Time Feels Like Your Enemy
Time management skills are essential to overall health and well-being, including combating stress [17]. Strong time management helps create a better work-life balance, so you don't spend your free time playing catch-up [17]. Proper implementation of these skills makes work easier and allows nurses to perform tasks more intelligently [18].
Time management training enhances nurses' knowledge of these skills, reducing the time required for various tasks [18]. Nurses make good use of the limited time in a work shift by learning to:
- Prioritize tasks effectively
- Plan operational activities
- Delegate tasks in non-specialist cases
- Manage communication with patients and colleagues
- Manage sessions efficiently [18]
Effective management results in increased patient and nurse satisfaction [18]. It enables nurses to spend more time with patients and get to less urgent nursing tasks that remain important [19]. Taking breaks lowers your risk of on-the-job injury and of making errors [19]. Breaks also help reduce fatigue and burnout [19].
Making Self-Care Non-Negotiable (Not Optional)
Self-care is the daily process of being aware of and attending to your basic physiological and emotional needs. It serves as the foundation for physical and emotional wellness to prevent mental health, occupational, or educational burnout [20]. The Nursing Code of Ethics actually codifies self-care, establishing that nurses have a moral responsibility to meet their own physical, emotional, mental, and spiritual needs [21].
Let that sink in. It's not selfish. It's your professional responsibility.
Professional nurses employed in healthcare settings struggle to maintain a balance between professional demands and self-care practices, which negatively affects their well-being [22]. Healthcare organizations must assist professional nurses in incorporating self-care practices into their daily routine [22]. Self-care reduces stress, replenishes a nurse's capacity to provide compassion and empathy, and helps improve the quality of care [23].
The basics matter: adequate sleep, healthy eating, and physical activity contribute to self-care practices [22]. Professional nurses struggle with self-care practices primarily because they lack time to engage in basic activities [22]. Working overtime disrupts normal sleeping patterns [22]. Stopping overtime work provides more time for oneself and better-quality sleep [22].
I get it. Finding time feels impossible when you're barely keeping your head above water. But here's the truth I've learned through my own struggles and countless conversations with healthcare workers: you can't pour from an empty cup.
Your patients need you to be healthy. Your family needs you to be present. You deserve both.
Micro-Wellness Stuff That Actually Works During Your Shift

Image Source: Health eCareers
What I Mean by Micro-Wellness (And Why It Matters)
When I speak at nursing conferences, I always ask the audience: “How many of you have time for hour-long yoga classes during your 12-hour shifts?”
The laughter tells me everything I need to know.
That's why I focus on micro-wellness practices – brief self-care interventions that take minimal time but fit into the chaos of nursing shifts. The NURSE acronym offers five micropractices that I've seen work: Notice (without judgment), Unconditional (self-compassion), Response (adaptive reactions), Strengths (building resilience), and Empower (physical actions) [13].
Here's what's cool about this: even brief mindfulness self-care strategies actually reduce stress intensity and help you develop better responses to perceived threats [13]. When you practice these regularly throughout your shift, they add up to several minutes and genuinely promote well-being [13].
The key is making them so simple that you can't talk yourself out of doing them.
Chair Yoga That Won't Get You Weird Looks
I get it – you're not doing downward dog in the middle of the ICU. But these moves? You can do them anywhere without it looking like you're having a breakdown.
Yoga improves your lymphatic and metabolic health while developing body awareness [13]. The Tree pose builds core strength in seconds: stand with feet shoulder-width apart, take a slow, deep breath while lifting your hands overhead, lift your heels off the floor if you're feeling it, hold for a few seconds, then bring your arms down while exhaling [13].
Shoulder rolls are my personal favorite for tension relief – roll those shoulders up, back, and down three or four times [24]. Side bends stretch your neck by just dropping your ear to one shoulder and taking a breath or two [24]. All of these take about 30 seconds [24].
Quick Decision-Making Tools I Recommend at Conferences
At nursing conferences, I always recommend courses on one-minute leadership tools that help with quick decision-making during high-pressure situations. These brief interventions support better clinical judgment without requiring extended time away from patient care.
Because sometimes you need to make a critical decision, and your brain feels like mush.
Mental Resets That Take Zero Extra Time
The beauty of these techniques is that they happen during stuff you're already doing. Hydration breaks with intention, quick stretches at the nurses' station, and mindful moments during medication scans provide mental resets [25].
Instead of scrolling on your phone between patients, take a five-minute digital detox by closing your eyes or gazing out a window to reduce mental fatigue [25]. Trust me on this one – your brain needs the break more than you need to check Instagram.
Here's one of my favorite hacks that I mentioned earlier: transform routine moments like handwashing into mindfulness opportunities through mini body scans [26]. You're washing your hands anyway – might as well reset your nervous system while you're at it.
Some nurses I know keep aromatherapy sticks stashed in their pockets for instant stress relief [27]. Peppermint works wonders when you feel like your head's about to explode.
The point isn't to add more to your already overwhelming day. The point is to work with what you're already doing and make it work better for you.
Getting Real About Mental Health Support That's Actually Available
When I speak at nursing conferences, I always ask how many people know about their Employee Assistance Program. Usually, about half the room raises their hands. Then I ask how many have actually used it. Maybe five percent.
That's a problem, because these programs exist specifically to help you through the exact challenges that cause burnout.
What Employee Assistance Programs Actually Offer
Employee assistance programs provide voluntary, confidential support for life challenges that mess with your job performance, health, and personal well-being [28]. Most offer up to 6 free counseling sessions [28]. They handle stress, money problems, legal issues, family drama, workplace conflicts, and substance use disorders [28].
Here's something that might surprise you: the productivity improvement from a single employee using an EAP can be worth $15,600 annually [29]. That's not just good for you – it's good for your organization too.
How to Actually Access Support Without Career Worries
Most healthcare organizations provide EAP services through HR or benefits departments [30]. These services stay confidential and run 24/7, 365 days a year [31].
I get it – you might worry about accessing mental health support affecting your career. The reality is these programs are staffed with professionals who understand healthcare work [12]. You can use these services without worrying about your career.
Sometimes talking with a peer who gets your daily reality helps most [12]. Other times, you need professional mental health support [12]. Both options exist, and both stay confidential.
Crisis Support That Actually Works
Crisis support runs continuously. Call or text 988 to connect with trained crisis counselors [11]. Safe Call Now offers confidential support at (206) 459-3020 [32]. Crisis Text Line responds when you text BADGE to 741-741 [32]. NAMI helps you find services at 800-950-6264, Monday-Friday 9 am-5 pm [11].
Training That Makes Sense for Your Schedule
The American Nurses Foundation partnered with pilot sites to adapt the Stress First Aid curriculum specifically for nurses [33]. You can access it for free through their Learning Management System [33]. The training covers evidence-based mental health care and professional well-being [34].
The point is this: support exists. It's confidential. It's designed for people who do what you do. You just have to use it.
Why Professional Growth Matters More Than Most People Think
Through my work speaking at nursing conferences and healthcare organizations, I've noticed something interesting. The nurses who seem most resilient – the ones who aren't completely burned out – they're usually the ones still learning, still growing professionally.
Access to professional development opportunities helps manage burnout while encouraging nurses to strive for career growth [35]. I see this firsthand when I present at conferences. Training and education are directly linked to nurses' career satisfaction [35]. Programs that promote specialization, certification, or advanced degrees reignite nurses' passion for their work, enhancing engagement and reducing the likelihood of burnout [15]. When organizations invest in ongoing education, they're really investing in their nurses' well-being [15].
Conferences That Actually Matter (And Why You Should Go)
Here's what I tell nurses about conferences: they're not just about the CEUs.
Nursing conferences offer powerful opportunities to learn what's new in healthcare, sharpen clinical skills, and connect with other nurses [10]. The energy at these events reminds me why I love this work. The American Organization for Nursing Leadership Conference attracts over 4,000 attendees annually and features over 50 speakers [10]. The ANCC National Magnet Conference brings together nurses and healthcare stakeholders from around the world [10]. The NBNA Institute and Conference hosts over 1,200 nurses and nursing students with over 100 exhibitors [10].
When I speak at conferences, I watch nurses light up when they realize they're not alone in their struggles. That connection matters.
Finding Mentors and Becoming Leaders
Another thing I've learned from presenting to nursing groups: every nurse needs someone in their corner.
Leadership development is critically important for the nursing profession [36]. Formal leadership training programs build leadership knowledge and skills [36]. But more than that, tailored leadership mentoring increases self-confidence in leadership [36]. Mentorship promotes engagement, retention, and connection [7]. Over 500 unique participants achieved an 87% two-year retention rate through structured mentorship programs [7].
I've watched nurses transform when they find the right mentor – someone who believes in them and helps them see possibilities they couldn't see before.
Planning Your Path Forward
Career pathways foster personal and professional growth by providing a clear roadmap [16]. The numbers don't lie: hospitals with professional development programs experienced a 34% decrease in nurse turnover rates [16]. Career pathways help combat the nursing shortage [16].
But here's what the statistics don't capture: flexibility to pivot your career or change specialties prevents burnout and leads to a fulfilling career [37]. Some of the happiest nurses I meet are the ones who've switched specialties, gone back to school, or found new ways to use their skills.
Your career doesn't have to be a straight line. Sometimes the detours are what save us from burnout.
What Organizations Actually Need to Change (And Why Individual Fixes Aren't Enough)
Staffing Ratios Matter More Than We Want to Admit
Here's what I've learned from presenting at healthcare organizations: you can teach nurses all the breathing techniques in the world, but if they're drowning in patient assignments, none of it matters.
The data doesn't lie. Each additional patient per nurse increases the likelihood of mortality within 30 days of admission by 7% and raises burnout odds by 23% [39]. That's not just a statistic – that's someone's mother, father, or child. And it's someone's career-ending because the system failed them.
California figured this out in 2004 when it mandated maximum staffing levels – no more than five patients per nurse on medical-surgical units [39]. Even safety net hospitals operating on tight budgets found ways to make it work [40]. If California can do it, other states can too.
I've seen the difference adequate staffing makes during my hospital visits. Nurses move differently when they're not constantly in crisis mode. They have time to actually connect with patients instead of just checking boxes.
The Break Policy Problem Nobody Talks About
Thirty percent of nurses rarely or never take 30-minute rest breaks [41]. THIRTY PERCENT.
Think about that for a second. We wouldn't ask marathon runners to skip water stations, but we expect nurses to work 12-hour shifts without proper breaks. The human body isn't designed for that kind of sustained stress.
California's S.B. 1334 guarantees enforceable breaks for public-sector workers – if employers don't provide breaks, they pay an additional hour at the regular rate [14]. That's real accountability. Workers on evening and night shifts had poorer sleep quality and shorter duration than day shift workers, potentially needing additional or longer breaks [8].
Through my conversations with nurses, I've learned that many feel guilty taking breaks because it means their colleagues pick up the slack. That's a system problem, not a personal failing.
Policy Changes That Actually Protect Nurses
Nurses should be protected from practices that promote excessive fatigue, such as mandatory overtime exceeding 12 hours daily or 60 hours weekly [40]. Period. No exceptions. No “but we're short-staffed” excuses.
Healthcare organizations need to establish standards, monitor them, and create processes to address problems when they find them [40]. This isn't rocket science. It's basic human resource management.
Measuring What Matters (Beyond Just Patient Satisfaction Scores)
Organizations need to include well-being measures, such as burnout rates and intent to leave, in their core quality metrics [42]. If you're not measuring it, you're not managing it.
I recommend that healthcare systems hire dedicated Chief Wellness Officers to spearhead planning and communicate directly with leadership [42]. Someone needs to own this problem at the executive level. Conduct regular assessments annually and share results across practices and departments [42].
The bottom line? Individual resilience training is important, but it's not enough on its own. Systemic problems require systemic solutions. We can't meditate our way out of unsafe staffing ratios.
What Actually Works: My Take on These Strategies
I've seen enough nursing conferences and talked with enough exhausted healthcare workers to know that not all burnout advice is created equal. Here's what I've learned actually makes a difference:
The stuff that works immediately:
- Those 30-second breathing techniques aren't just feel-good fluff. I've watched nurses use the 4-7-8 reset between patient rooms and seen the difference it makes.
- Micro-wellness practices during shifts (the NURSE acronym, chair yoga, mindful handwashing) – these actually fit into real nursing workflows.
- EAP programs that offer 24/7 confidential support. The productivity improvement can be worth $15,600 per employee annually, which should get administrators' attention.
The stuff that takes time but changes everything:
- Peer support programs like EmBRACE that match you with someone who actually understands your daily reality. Depression decreases, empowerment increases.
- Transformational leadership that gives you autonomy instead of micromanaging every decision.
- Professional development opportunities that remind you why you became a nurse in the first place.
The systemic changes that hospitals hate to hear about:
- Mandated staffing ratios. Each additional patient per nurse increases your burnout odds by 23% and patient mortality by 7%.
- Enforceable break policies. Thirty percent of nurses rarely or never take their 30-minute rest breaks, which is insane.
- Chief Wellness Officers who actually have authority to make changes, not just organize wellness fairs.
What I tell nurses at conferences: The individual techniques matter – you need tools for surviving your shifts. But if your hospital won't address the root causes like unsafe staffing and impossible patient loads, those breathing exercises will only take you so far.
The most honest feedback I get is that nurses want both: practical skills they can use today AND organizations that actually give a damn about their wellbeing. When you have both working together, that's when nurses can sustain their passion for patient care without destroying themselves in the process.
The bottom line: Some strategies work in 30 seconds. Others require organizational commitment. The nurses who thrive in the long term have access to both.
Conclusion
Nurse burnout represents a workforce crisis requiring both individual tools and systemic solutions. Given that frontline nurses constantly operate in high-stress environments with elevated cortisol levels, quick interventions such as two-minute self-care practices, chair yoga, and brief meditations are essential during shifts, not just on days off. My conversation with that nurse at my annual physical reinforced why this work matters. When nurses have practical stress management tools, they can bring their best energy to patient care. Healthcare organizations must pair these individual strategies with institutional changes, such as fair staffing ratios and supportive leadership. Overall, nurses deserve resources that actually work in real-world clinical settings.
FAQs
Q1. What exactly is nurse burnout, and how is it officially defined? Nurse burnout is recognized by the World Health Organization as an occupational phenomenon characterized by three key dimensions: feelings of exhaustion or energy depletion, increased mental distance from one's job with feelings of cynicism, and reduced professional effectiveness. It results from chronic workplace stress that hasn't been successfully managed and applies specifically to work contexts rather than other life areas.
Q2. What are some quick stress relief techniques nurses can use during their shifts? Nurses can practice the 4-7-8 Reset breathing technique (inhale for 4 counts, hold for 7, exhale for 8), which takes just 30 seconds and activates the parasympathetic nervous system. Other effective methods include two-minute body scans, mindful handwashing for 30-60 seconds, chair yoga stretches, and the STOP technique (Stop, Take a breath, Observe, Proceed). These micro-wellness practices require minimal time but create measurable physiological changes.
Q3. How does work-life balance impact burnout rates among nurses? Over 60% of nurses globally experience poor work-life balance, which directly contributes to increased stress, burnout, and job dissatisfaction. Research shows that work-life balance is directly proportional to job satisfaction and inversely proportional to psychological distress. When nurses achieve equilibrium between their professional and personal lives, they report reduced stress, improved mental health, and higher job satisfaction.
Q4. What role do Employee Assistance Programs play in supporting nurses' mental health? Employee Assistance Programs offer confidential, free support services typically including up to 6 counseling sessions, available 24/7 year-round. These programs address stress, family problems, substance use disorders, and other challenges affecting job performance and well-being. The marginal productivity improvement from a single employee using an EAP can be as high as $15,600 annually, and services remain completely confidential without career implications.
Q5. How do staffing ratios affect nurse burnout and patient outcomes? Lower nurse-to-patient ratios directly correlate with reduced burnout and better patient outcomes. Research shows that each additional patient per nurse increases the likelihood of mortality within 30 days of admission by 7% and raises the odds of nurse burnout by 23%. California's mandated maximum of five patients per nurse on medical-surgical units demonstrates that systemic staffing improvements are achievable even in safety net hospitals.
References
[1] – https://www.nursingworld.org/content-hub/resources/workplace/what-is-nurse-burnout-how-to-prevent-it/
[2] – https://www.who.int/news/item/28-05-2019-burn-out-an-occupational-phenomenon-international-classification-of-diseases
[3] – https://www.usa.edu/blog/nurse-burnout/
[4] – https://www.connectrn.com/blog/burnout-in-2026-looks-different
[5] – https://briviohealth.com/2026/03/nurse-burnout-solutions-health-systems/
[6] – https://pmc.ncbi.nlm.nih.gov/articles/PMC7862989/
[7] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12013355/
[8] – https://wifitalents.com/nurses-burnout-statistics/
[9] – https://pmc.ncbi.nlm.nih.gov/articles/PMC7599295/
[10] – https://www.phoenix.edu/articles/nursing/nurse-burnout-symptoms-recovery-and-prevention.html
[11] – https://www.aiam.edu/nursing/nurse-burnout-symptoms/
[12] – https://www.nurse.com/blog/common-nurse-burnout-symptoms-nsp/
[13] – https://www.who.int/news/item/25-04-2024-202404_protecthw_mentalhealth
[14] – https://aanmc.org/naturopathic-medicine/stress-management-healthcare-professionals/
[15] – https://www.cdc.gov/niosh/healthcare/risk-factors/stress-burnout.html
[16] – https://sereneprimarycare.com/informed-empowered/the-science-backed-guide-to-2-minute-stress-relief-micro-meditations-that-actually-work
[17] – https://www.steadymd.com/blog/8-ways-to-relieve-stress-in-2-minutes-or-less/
[18] – https://www.shiftmed.com/professionals/blog/mindfulness-techniques-to-help-nurses-manage-stress/
[19] – https://pmc.ncbi.nlm.nih.gov/articles/PMC11999806/
[20] – https://www.aonl.org/mindfulness-may-help-nurses-build-resilience
[21] – https://www.elitelearning.com/resource-center/nursing/nursing-resources/self-care-nursing/4-simple-stress-relieving-exercises-for-nurses/
[22] – https://nursing.buffalo.edu/news-events/nurses-report.host.html/content/shared/nursing/articles/nurses-report/posts/self-care-tips.detail.html
[23] – https://www.nurse.com/blog/tame-nurse-stress-mindfulness-meditation/
[24] – https://consultqd.clevelandclinic.org/mindfulness-practices-help-even-the-busiest-nurses-de-stress
[25] – https://www.myamericannurse.com/self-care-during-a-single-shift/
[26] – https://pmc.ncbi.nlm.nih.gov/articles/PMC11959789/
[27] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12677997/
[28] – https://www.sciencedirect.com/science/article/abs/pii/S1541461220300926
[29] – https://www.myamericannurse.com/peer-support-and-nurse-well-being/
[30] – https://aacnjournals.org/ajcconline/article/34/5/335/32828/Registered-Nurses-and-Meaningful-Recognition
[31] – https://www.aacn.org/nursing-excellence/healthy-work-environments/meaningful-recognition
[32] – https://www.nursingworld.org/content-hub/resources/nursing-leadership/nurse-recognition/
[33] – https://www.ahrq.gov/hai/cusp/modules/implement/teamwork-notes.html
[34] – https://www.ncbi.nlm.nih.gov/books/NBK2637/
[35] – https://online.umn.edu/story/6-reasons-effective-communication-matters-health-management
[36] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12530567/
[37] – https://pmc.ncbi.nlm.nih.gov/articles/PMC11646404/
[38] – https://nursingeducation.org/insights/professional-boundaries/
[39] – https://online.hpu.edu/blog/professional-boundaries-in-nursing
[40] – https://www.nursemagic.ai/post/how-to-set-boundaries-as-a-nurse-without-compromising-patient-care
[41] – https://www.nursingworld.org/content-hub/resources/workplace/time-management-tips-for-nurses/
[42] – https://pmc.ncbi.nlm.nih.gov/articles/PMC9184972/
[43] – https://online.regiscollege.edu/blog/nurse-time-management-techniques-and-tips
[44] – https://www.aacnnursing.org/5b-tool-kit/themes/self-care
[45] – https://absn.ndm.edu/blog/self-care-for-nurses/
[46] – https://pmc.ncbi.nlm.nih.gov/articles/PMC12817031/
[47] – https://www.purdueglobal.edu/blog/nursing/self-care-for-nurses/
[48] – https://pmc.ncbi.nlm.nih.gov/articles/PMC9595406/
[49] – https://consultqd.clevelandclinic.org/nurses-yes-to-yoga-even-at-work
[50] – https://www.healthecareers.com/career-resources/nurse-wellbeing/micro-self-care-for-nurses-simple-habits-to-recharge-and-thrive
[51] – https://www.wisconsinnurses.org/redefining-nurse-wellness-beyond-bubble-baths-and-yoga-mats/
[52] – https://nurse.org/articles/employee-assistance-program/
[53] – https://allonehealth.com/employee-assistance-programs-for-healthcare-workers/
[54] – https://www.hca.wa.gov/about-hca/programs-and-initiatives/washington-wellness/employee-assistance-program-eap
[55] – https://www.hhs.gov/about/agencies/asa/foh/bhs/employee-assistant-program/index.html
[56] – https://www.nami.org/frontline-professionals/health-care-professionals/
[57] – https://www.dhs.state.il.us/page.aspx?item=172735
[58] – https://responderstrong.org/
[59] – https://www.nursingworld.org/foundation/programs/nurse-wellbeing/curriculum/
[60] – https://drlornabreen.org/allinformentalhealth/six-actions/mental-health-education-training/
[61] – https://www.indwes.edu/articles/2025/06/preventing-nurse-burnout
[62] – https://www.ache.org/blog/2025/addressing-nursing-burnout
[63] – https://nurse.org/articles/must-attend-nursing-conferences/
[64] – https://www.sciencedirect.com/science/article/pii/S0029655424001866
[65] – https://www.aacn.org/blog/a-recipe-for-nurse-mentorship-programs
[66] – https://pmc.ncbi.nlm.nih.gov/articles/PMC10254089/
[67] – https://www.nursingworld.org/content-hub/resources/becoming-a-nurse/nursing-career-pathways/
[68] – https://ldi.upenn.edu/our-work/research-updates/how-inadequate-hospital-staffing-continues-to-burn-out-nurses-and-threaten-patients/
[69] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8769498/
[70] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8447039/
[71] – https://www.weintraub.com/2022/10/meal-and-rest-periods-for-public-healthcare-workers-now-guaranteed/
[72] – https://www.cdc.gov/niosh/work-hour-training-for-nurses/longhours/mod5/10.html
[73] – https://www.ama-assn.org/practice-management/physician-health/6-steps-measuring-physician-burnout-and-then-reversing-it

